The next level drug is generally Prolia, the monoclonal antibody denosumab, given by injection every six months -which slows bone loss by preventing the formation of the bone-dissolving osteoclasts. Bisphosphonate drugs also have a small risk of side effects that include fractures of the femur and bone decay in the jaw. GI issues can arise during the strict regimen involved in taking bisphosphonate pills such as Fosamax: once a week, first thing in the morning, on an empty stomach-followed by sitting or standing upright for at least 30 minutes before eating. The first-choice drug treatment is usually bisphosphonates –which can slow bone breakdown by blocking the osteoclasts, in turn allowing osteoblasts to create more new bone. Of the various forms of bisphosphonates, including pills and injectable medication, my doctor recommended yearly infusions of zoledronic acid (Reclast), preferred for anyone who has had acid reflux, also known as heartburn, when stomach acid backs up into the esophagus and irritates the tissue.
For higher level drugs like Prolia, early research suggested that stopping the medication risked causing greater bone loss, but recently women with sufficiently improved T-scores have been able to go off medication entirely or move to less powerful drugs. Osteoporosis drug treatment typically lasts two to five years-because longer regimens can increase the risk of side effects and because improvements in bone strength by that time can prolong bone-protective effects after stopping the medication. With all this information, my rheumatologist used a “ 10-Year Fracture Risk Calculator” that placed my “risk of any fracture” at 26%-in the red danger zone on the chart, compared to the average for my age of 15%.
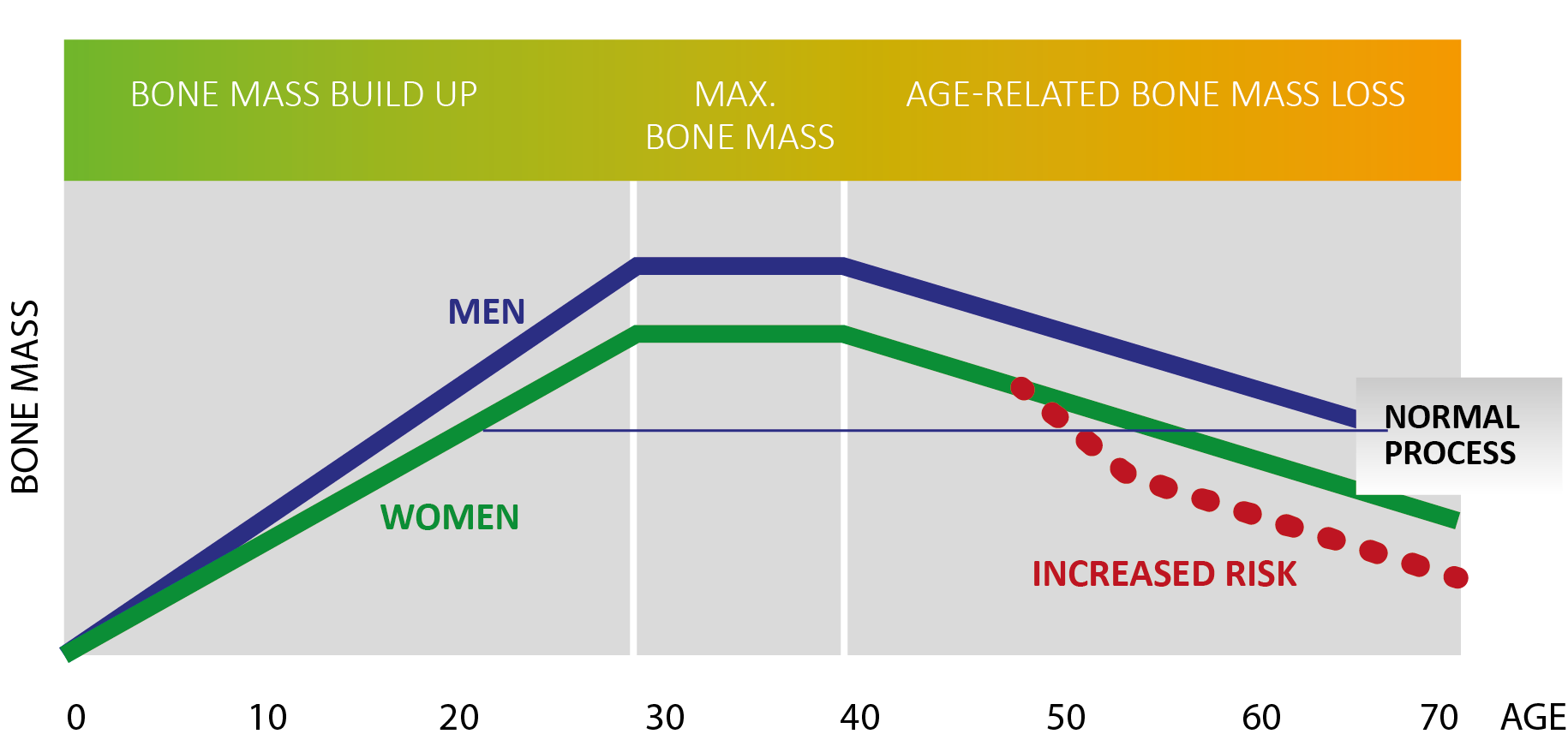
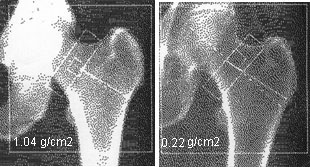
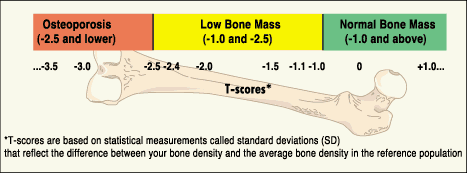
Among less clear risk factors, my mother’s health was generally too poor to say what caused what and my lifestyle habits like eating and exercise are pretty good. But adding my age, weight and race indicates higher risk, as does a broken kneecap from a fall several years ago. My -2.4 T-score is borderline, officially labeled osteopenia, which can signal problems ahead but is not itself cause for treatment. For women as a group, T-scores of -2.5 or below indicate a 33% chance of fracturing a hip compared with a 16% risk for those with a score of -1, the average for a 30-year-old woman. In addition, studies showing benefits of calcium/vitamin D supplements at that time had not been controlled but observational, and they failed to assess diet, exercise and other important variables. Prescription drug treatment decisions began with my T-score, the measurement of bone mineral content by a DEXA or DXA scan -as an indication of bone density or strength. By contrast, in 2019, research from the NHANES study involving more than 30,000 American adults linked vitamin D supplements of more than 400 IU/day a study with “an increased risk of death from cancer” and “increased cancer death and death from any cause,” according to the New York Times. For the 700mg still needed, calcium supplements should total 350mg twice a day.įor vitamin D, she advised 1,000 IU/day. Determination of supplement amounts, however, required first measuring and subtracting dietary intake: for me, about 300mg from milk and cheese and maybe 200mg more from orange juice, a few vegetables and ice cream. Her recommended dose for calcium, advising not to take less or more, was 1,200 mg-ingested over the course of each day, in at least two separate doses to maximize use by the body. My new rheumatologist provided clarity and specificity, updated. government- appointed panel of physicians recommended “against daily supplementation” with vitamin D and calcium, while my internist advised stopping both, and my gynecologist recommended maximum doses.ĭiminishing bone density occurs over time when bone resorption exceeds bone formation-which is controlled by hormones, such as estrogen and parathyroid hormone, as well as by specific proteins in the bone: osteoblast cells create new bone while osteoclasts break it down. (Note: for all recommendations made below, readers should check with their personal physicians.)Īt the time of the 2019 post, a U.S. AFTER WRITING two previous posts (2014, 2019) on women who might be at risk for osteoporosis, Mary Carpenter’s new Georgetown University rheumatologist provided updated numbers on risks and needs for supplements and drug treatment, and a new focus on other issues.
